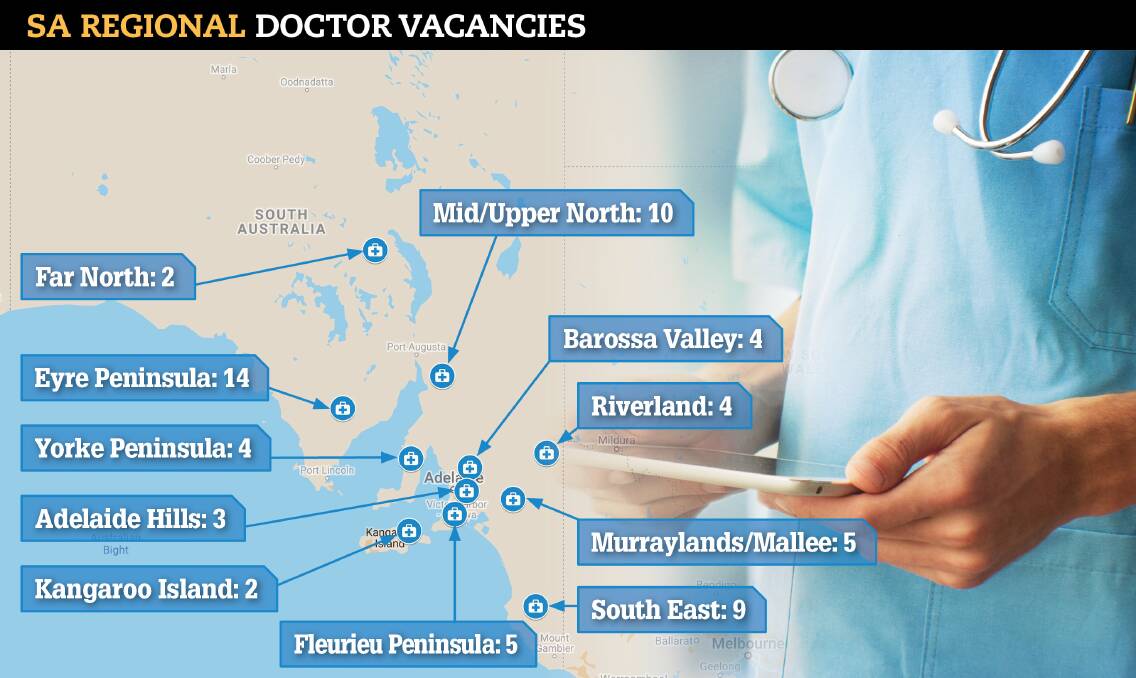
THE state government has released its draft plan to attract more doctors and medical staff to work in rural areas, with the announcement coming while more than 60 general practitioner job vacancies are advertised across regional SA.
There are 62 jobs advertised on the Rural Doctors Workforce Agency, with the Eyre Peninsula the greatest region in need at 14 vacancies.
The plan to recruit, train and develop medical staff for regional SA was developed as part of the government's Rural Health Workforce Strategy, which has a budget of $20 million until 2022, including $2.9m this financial year.
Among the proposals put forward in the draft plan are expanding intern and resident training capacity in rural hospitals, providing a pathway for future rural GPs, an audit of training capacity in regional areas and preparation for a national rural generalist training pathway.
Research from Flinders University, in partnership with National Rural Health Commissioner Paul Worley, has shown that a training pathway needs to be developed for rural doctors. This is one of the tasks taken up by Emeritus Professor Worley.
"Rural communities need doctors that can provide comprehensive GP, emergency and other specialist services that would ordinarily be delegated to other doctors in the city," he said.
Prof Worley said a specific training pathway would ensure regionally-based doctors would meet the breadth and width of a rural community's needs.
"There is a significant number of doctors who have been enthused about rural practice in our state's two medical schools," he said.
"The presence of a clearly articulated and supported pathway will encourage others who may have been on the fence about rural practices to see it as a high status, viable and rewarding career."
Prof Worley, who practices as a doctor at Yankalilla, said working in rural areas was a "fantastic" opportunity.
"Rural practices offer more variety than any other form of medicine," he said.
"This is cradle to grave medicine, hospital and community health, a combination of high tech and close relationships."
Prof Worley said the recent $62.2m allocated to the implementation of a National Rural Generalist Pathway in the federal budget meant progress was imminent.
"From where I sit, both levels of government are ready to work together," he said.
He emphasised training for the pathway needed to be located across rural SA.
RELATED READING: Rural SA suffering doctor shortage
Other options considered in the draft plan were expanding the number of nurse practitioners in rural emergency departments and investigating provisions for practice nurses to provide on-call cover to rural public hospitals.
Rural practices offer more variety than any other form of medicine.
- PAUL WORLEY
Health and Wellbeing Minister Stephen Wade said there were 35 vacancies in SA's GP training program, all in regional areas.
"These vacancies affect both the services we can offer and the future GP workforce supply," he said.
RDWA chief executive officer Lyn Poole said while the 62 doctor vacancies were the highest they had been in her recollection, the story was not all bad.
"A large number of these are thriving practices that could have extra people in bigger communities," she said. "Our focus and priority is on EP and a couple of spots in the Mallee.
"These are smaller communities that can have trouble attracting doctors."
Ms Poole said despite RDWA working alongside national recruiters to try and fill these roles, the problem remained.
"That tells me the market is really flat," she said.
"We don't have towns with no doctors, but we have towns with inadequate service."
Ms Poole said about 1500 people undertook GP training each year, with half on the rural pathway.
"The question of volume is not the issue, rather the issue is of distribution," she said.
Ms Poole said it was important to "get the right people in the right place", which meant doctors in these smaller towns needed to have a high level of skills, while larger centres, such as Mount Gambier, were better placed to help train junior doctors.
"The issues we're facing aren't peculiar to SA, but SA is a bit different," she said. "In the eastern states, they've got a lot of larger regional centres, while we've got a lot of smaller communities. We're more akin to WA."
Ms Poole said there had already been good news for the medical workforce in Allied Health areas.
We don't have towns with no doctors, but we have towns with inadequate service.
- LYN POOLE
"Eight years ago you couldn't find a physiotherapist for love or money," she said. "The upside is that Allied Health is a faster path through university and into their own practice."
Member for Grey Rowan Ramsey said the situation had worsened in the past year since he wrote his discussion paper on the doctor shortage issue.
"Incumbent doctors are ageing and we're just not getting the replacements we need," he said.
Mr Ramsey said regions were largely dependent on internationally-trained doctors - "and thank goodness we can get those" - while there was still a reluctance for younger trainees to head to the bush.
He said there had been many strategies tried previously, including training located in regional areas, financial incentives and more, but there was still a preference to work in cities.
Mr Ramsey said statistics showed country residents accessed Medicare items at almost half the rate of those who lived in the city.
He said one option he had proposed was to issue postcode-specific Medicare provider numbers, which would link a doctor's ability to claim Medicare subsidies to their location.
"There are moves in that direction," he said.
Of the $2.9m allocated to the Rural Health Workforce Strategy this year, $840,000 has been designated to expanding the rural digital telehealth network to allow remote assistance for country clinicians, $180,000 for mental health education, $500,000 in various training schemes, $35,000 on workshops to show the benefits of rural dental careers and $7000 for part-funding of a promotional video aimed at high school and medical school students about the work and lifestyle opportunities of a career in rural medicine.
Community consultation on the draft plan begins on August 16.
- Details: sahealth.sa.gov.au/ruralhealthworkforce
- Start the day with all the big news in agriculture. Click here to sign up to receive our daily Stock Journal newsletter.


